TMR Theory and Hypothesis
2021, Volume 4 Issue 4
TMR Theory and Hypothesis,主要关注医学的理论研究和可行性假说分析,以开放的思维方式为医学提供新颖、激进的新想法和假设,为大多数传统期刊拒绝的激进假设开辟了新的领域,补充医学的理论内涵和现代化研究方法,促进医学理论研究的进步与发展。目前已被ScienceOpen,Ingenta Connect,J-Gate,中国科技期刊数据库(CSTJ),超星期刊数据库、Google学术搜索、知网空间、EuroPub收录。本刊特为优秀稿件开通快速发表的绿色通道,审稿1-2周,Online周期4周。

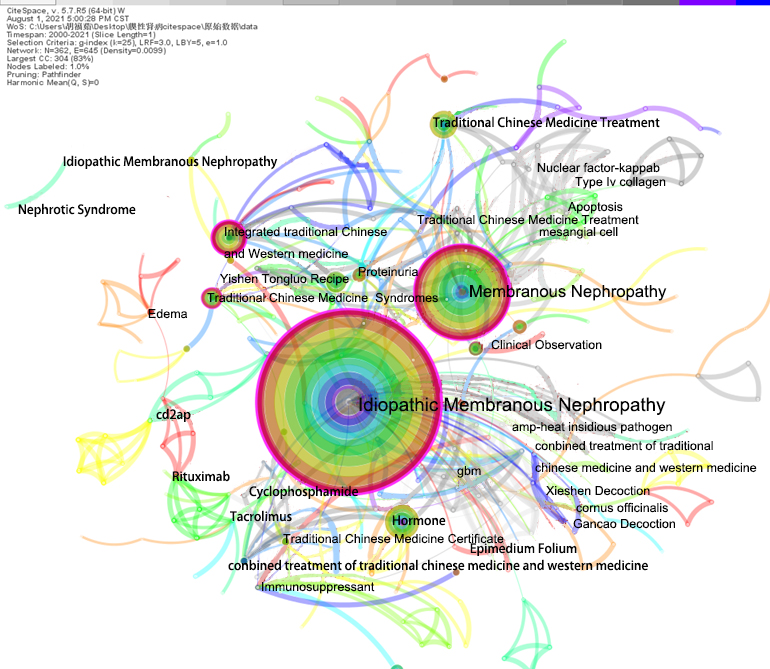
01 基于CiteSpace的特发性膜性肾病中医药研究现状与趋势的知识图谱分析
Objective: To analyze the current status and development trend of Chinese medicine research in the field of idiopathic membranous nephropathy since 2000. Methods: The literature related to Chinese medicine for idiopathic membranous nephropathy published in China Knowledge Network (CNKI) since 2000 was searched, and CiteSpacewas applied to visualize the publication time, authors, and keywords of the literature and to draw a visual knowledge graph. Results: 372 relevant literatures were included. Author analysis showed that there were 343 authors included, and the authors with the highest number of publications published 13 articles, and the core authors accounted for 10.2% of the total number; keyword analysis showed that 15 clusters were formed after burst analysis, and 10 emergent words were formed after keyword emergence analysis. Conclusion: Chinese medicine recognizes and intervenes in idiopathic membranous nephropathy in terms of evidence type, treatment method, common prescriptions and single herbs, auxiliary examination, treatment modality, and clinical research. The development trend lies in the combination of macroscopic and microscopic, the synergy between Chinese and Western, multidisciplinary collision diagnosis and treatment, as well as the use of Chinese medicine to intervene in the disease process at an early stage, and the integration of a worldwide standardized diagnosis and treatment guideline of Chinese medicine for idiopathic membranous nephropathy.
02 关于远距离外气疗法作用机制的假说
Distance External Qi Therapy (DEQT) is a form of Distance Intention Healing. Though it is getting popular, there is still no clear explanation on how it works. This article highlights the plausibility of supporting the mechanism of DEQT with the theory of quantum entanglement.

03 SARS-CoV-2 和胃肠道疾病
Since the 1918 influenza pandemic, the severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) has produced the largest pandemic throughout the globe. SARS-CoV and the Middle East respiratory syndrome (MERS-CoV) are both members of the Beta CoV. The coronavirus disease of 2019 (COVID-19) has terrible implications and is currently a serious health concern throughout the world. SARS-CoV-2 affects the respiratory system first since it is the major site of entrance into the patient, but it can also damage other systems. Aside from the typical respiratory problems, several COVID-19 patients develop gastrointestinal (GI) symptoms such as weight loss, vomiting, nausea, and diarrhea. SARS-CoV-2 may infect the GI system via the angiotensin-converting enzyme 2 (ACE2) receptor, and indications of a fecal-oral transmission pathway are growing. Globally, GI disorders (GIDs) are becoming a major source of morbidity in youth. The condition has a significant financial impact on healthcare systems and hurts people's lives; nonetheless, very little is documented about the condition's worldwide prevalence and incidence. Alterations in gut sensitivity, motility, microbiota, immunological function, and central nervous system processing are all factors that contribute to GIDs. GI malfunction results in changes in changes in gut bacteria as well as an elevation in inflammatory cytokines. As a result, recognizing GI symptoms that precede COVID-19 respiratory issues may be crucial for better early identification and treatment. In GI epithelial cells of the intestinal mucosa, ACE2 and transmembrane protease serine-type 2 were also discovered to be substantially expressed. SARS-CoV-2 may also infect and multiply in both GI and liver cells in a dynamic manner. These findings suggest that SARS-CoV-2 might be a viable target for the GI tract. This review focuses on the GI complications that arise due to COVID-19 and how the CoVs give rise to GI symptoms.
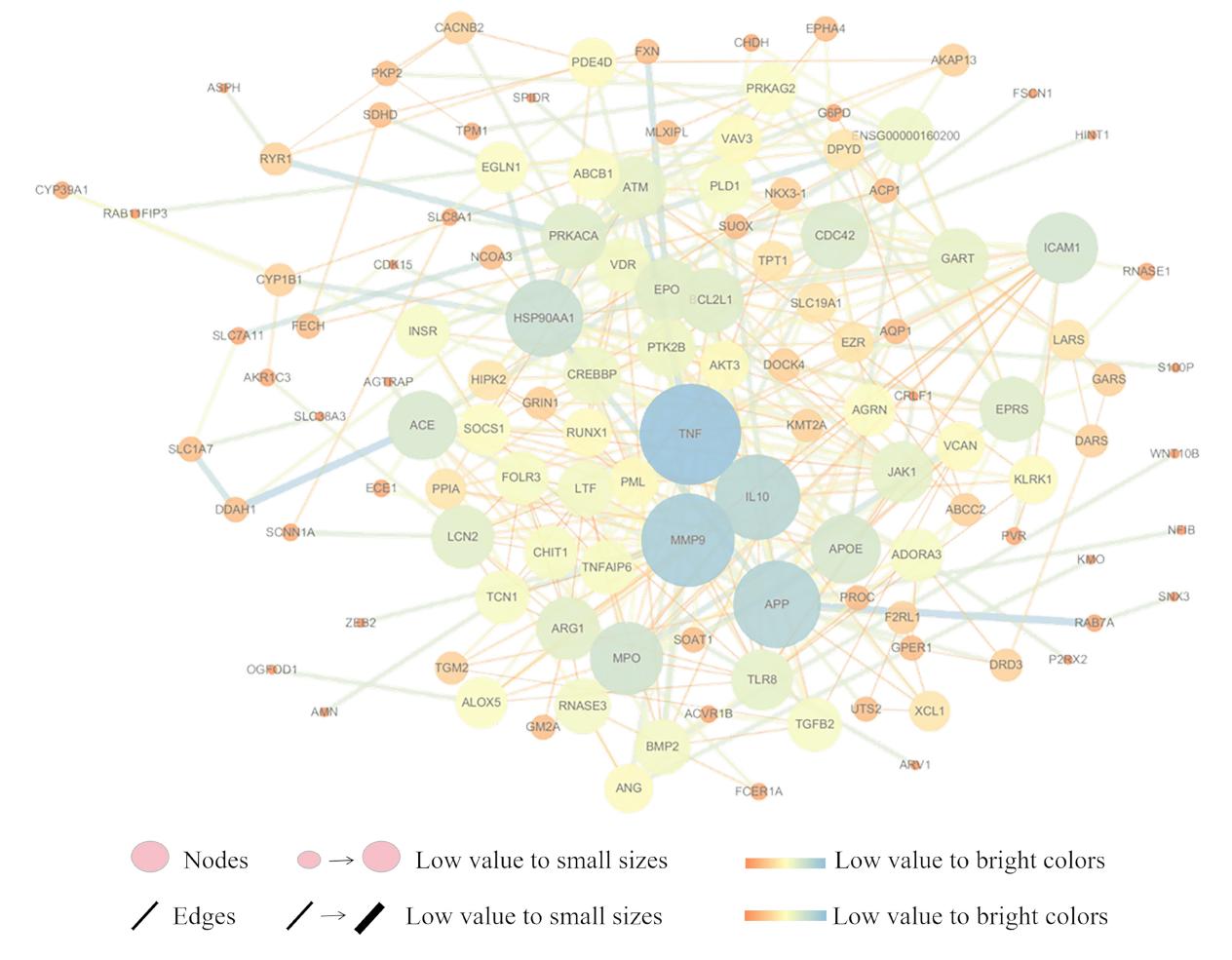
04 失眠颗粒(SMG)调节昼夜节律干预抑郁症的作用机理探索
Background: According to the World Health Organization, about 350 million people worldwide are suffering from depression. It's reported that depression has been linked to several circadian rhythm perturbations, suggesting a disruption of the circadian clock system in affective disorders. The present study investigates the possible molecular mechanism of Shimian granules (SMG) in treating depression via restoring disrupted circadian rhythms. Method: Firstly, network pharmacology approach was used to identify the compounds and potential targets of SMG in TCMIP and BATMAN-TCM database. Secondly, the differential expression genes were obtained by gene expression profiling in GEO database (GSE56931, GSE98793). Further, protein-protein interactions (PPI) network was used to screen out core targets by STRING v11. Moreover, functional enrichment was carried out in DAVID database. Conclusively, the "herbs-compounds-targets-pathways" network was established to explore the mechanism of SMG in the treatment of depression. Result: It was found out that 65 compounds, 18 targets and three pathways contributed to SMG in treating depression by regulating disrupted circadian rhythms, which might relate to core targets TNF, IL10, VDR in cAMP and calcium signaling pathway.Conclusion: Network pharmacology combined with gene expression profiling exhibited a powerful means to investigate the possible mechanism of formula, which contributes to theoretical basis for further study of SMG in the treatment ofdepression.
05 穴位埋线治疗产后肥胖伴胰岛素抵抗临床疗效探索
To observe the effect of catgut implantation at acupoints on the treatment of patients with postpartum obesity and insulin resistance. Methods: A total of 120 patients with postpartum obesity and insulin resistance were randomly divided into treatment and control groups (60 patients per group). The treatment group was administered catgut implantation at acupoints while the control group received acupuncture alone for 12 weeks. The patients’ body parameters, including body mass index (BMI), waist-to-hip ratio (WHR), fat percentage (FP), fasting blood glucose (FPG), fasting insulin (FINS), insulin resistance index (HOMA-IR), total cholesterol (TC), triglycerides (T), high-density lipoprotein (HDL-C), low-density lipoprotein (LDL-C), and other biochemical indexes of blood lipids, were compared before and after treatment to investigate the efficacy of catgut implantation and acupuncture on postpartum obesity with insulin resistance. Results: The overall response rates were 93.33% and 85% in the treatment and control groups, respectively. After treatment, BMI, WHR, FP, FINS, HOMA-IR, TC, TG, and LDL-C decreased, HDL-C increased (P < 0.05), and FPG did not change significantly (P > 0.05) in both groups; however, the changes in the treatment group were superior to those in the control group (P < 0.05). Conclusion: Both catgut implantation and acupuncture therapy showed good effects on improving postpartum obesity with insulin resistance. The therapeutic effect of catgut implantation on postpartum obesity was better than that of acupuncture therapy, and was therefore worthy of clinical application.